Diagnosing, treating and researching HIV-kala azar co-infection in Abdurafi – Ethiopia

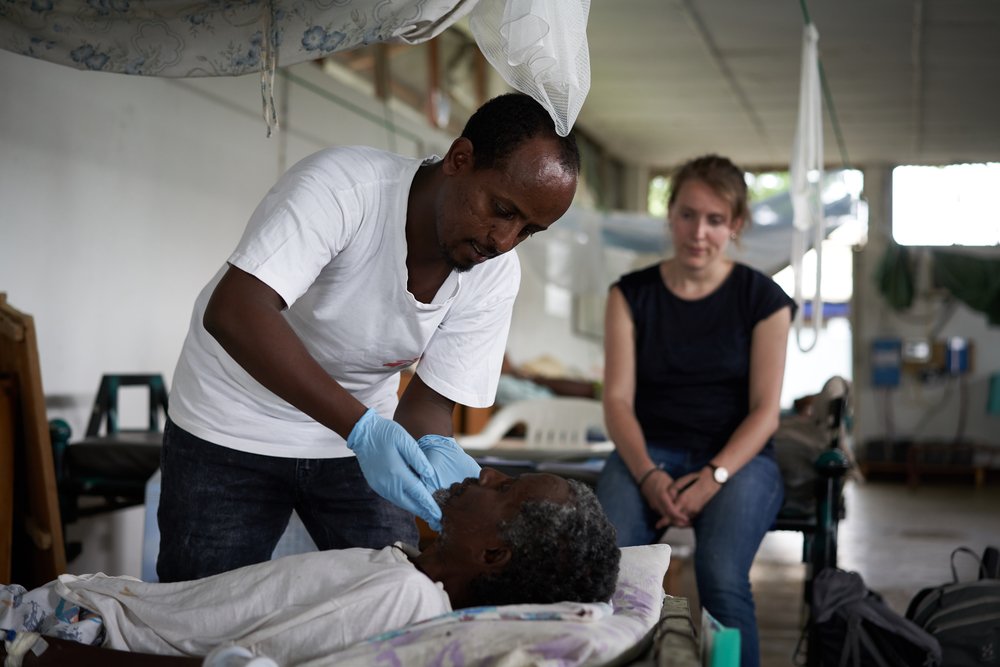
Kasaye sits on his bed in the intensive care unit of the MSF health centre in Abdurafi, a bottle of soda and some cookies in his hands. He looks incredibly frail and the simple acts of drinking and eating seem to require immense effort. “This is the thirteenth time that I have come to MSF for kala azar treatment,” he says. Kala azar (also known as visceral leishmaniasis) is the second largest parasitic killer after malaria, which makes it one of the most dangerous neglected tropical diseases in the world. Every year, it infects between 200,000 and 400,000 people mostly in Asia, East Africa and South America, and around 50,000 die because of it. “I was first diagnosed with the disease in 2002,” he continues. “I received treatment and the symptoms disappeared. I thought that I was cured,” he adds. Usually, once treated, patients become immune to the parasite. However, this was not the case for Kasaye who, one year later, was diagnosed with HIV. HIV can prevent patients from being fully cured of kala azar, exposing them to the risk of relapse. To make things more complicated, kala azar and HIV co-infection is disastrous because both conditions weaken the immune system and reinforce each other, leaving a person vulnerable to other opportunistic diseases like TB, malaria and dysentery. Ethiopia has a very high number of co-infected patients, with 20 to 40% of kala azar cases occurring in HIV positive people.
“During the years, I suffered from twelve other kala azar infections and the time between relapses is becoming shorter. I came to Amhara from Tigray as a migrant farm worker but kala azar has made me weak and I can’t work in the fields anymore. Now I live in the streets and I have no choice but to beg for money,” Kasaye says. Economic status seems to be a determining factor when it comes to kala azar relapse in HIV co-infected patients, as people in poor living conditions are more exposed to sandflies – the carrier of the parasite - and are further debilitated by the lack of food.
“Kala azar is endemic in the Abdurafi area and that’s why MSF decided to set up its intervention here,” says Dr. Ernest Nshimiyimana, medical team leader for the Abdurafi project. “In addition to providing treatment for kala azar and HIV, we also run a state of the art laboratory for the diagnosis of visceral leishmaniosis.”
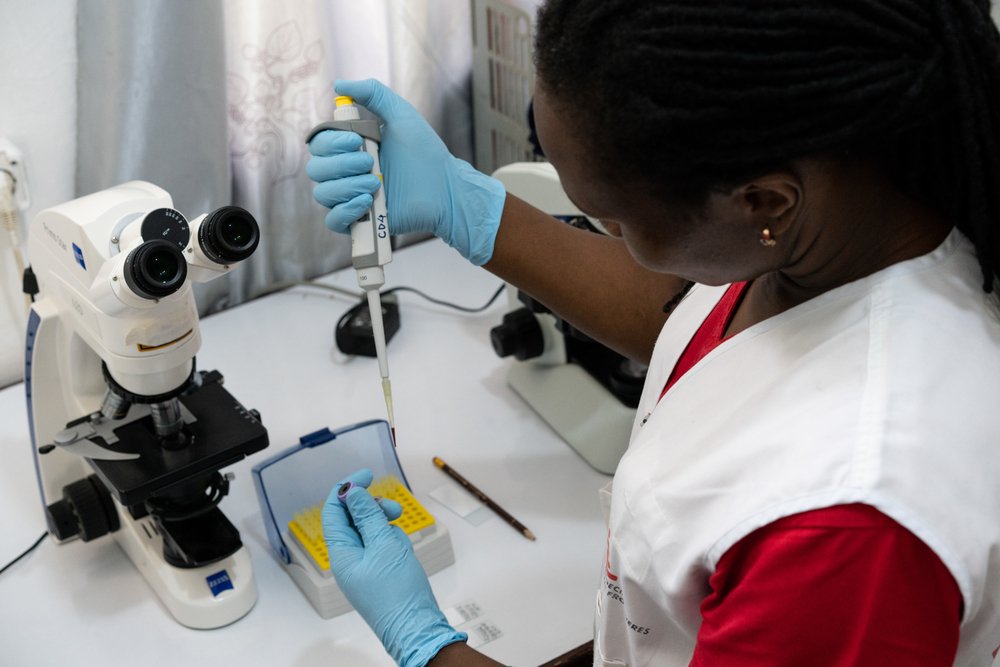
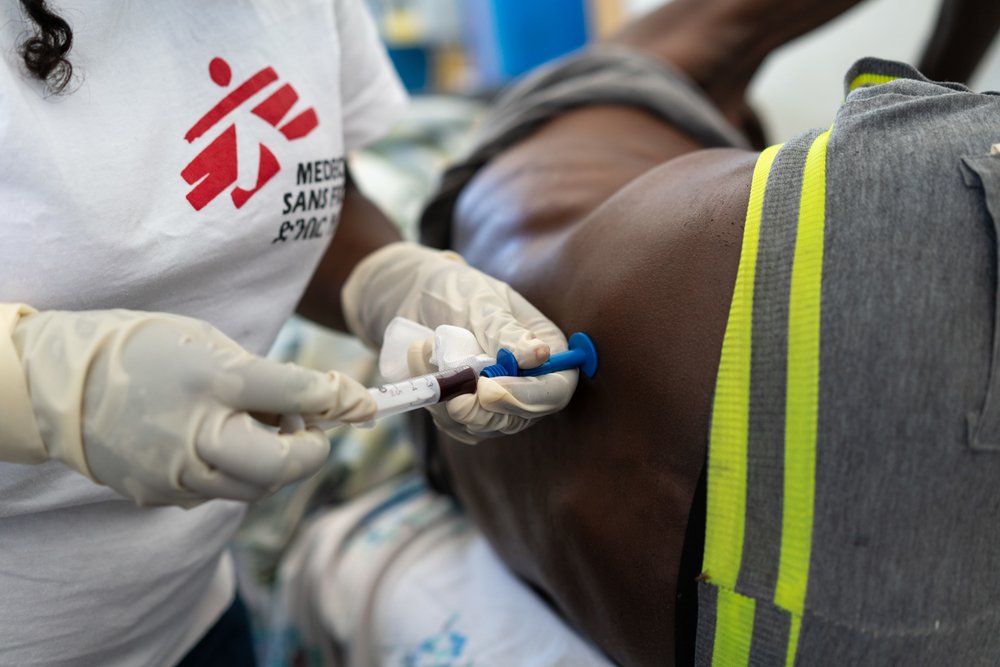
Diagnosing kala azar is a complicated matter. Rapid diagnostic tests are the diagnostic tool available in most health facilities, but they are reliable only with patients infected by kala azar for the first time (a condition called primary kala azar). “The MSF clinic in Abdurafi is one of the few places in Ethiopia where the presence of active kala azar parasites in a patient’s body can be accurately diagnosed,” continues Dr. Ernest. “To determine whether a patient is cured or not, or to diagnose kala azar in suspected relapse cases, a spleen or bone marrow biopsy is required. To analyze these samples, you need a specialized lab and here we have all the equipment we need.”
The importance of this lab is significant. Mortality rates are up to 14 times higher in HIV co-infected and relapse patients. Therefore, a timely diagnosis is instrumental in saving lives. “The majority of health facilities in the country do not have the tools or the expertise to carry on many of the tests that we can perform here. Some of them can also be very expensive, but MSF in Abdurafi offers all free of charge,” says Mercy Oluya, MSF lab manager. “We brought in experienced lab technicians and all the necessary equipment. We are also training the Bureau of Health staff that share the lab with us and perform all the other routine tests for our patients.”
The lab is also used to study the prevalence and incidence of kala azar in HIV patients in partnership with the Institute of Tropical Medicine Antwerp (ITM), the University of Gondar and the Ethiopian Regional Health Bureau in Amhara. Research began in October 2017 and will run for four years. Aderaju Kibret is MSF’s medical research manager and is responsible for the recruitment of patients for this study, as well as for the monitoring of their condition. “We are especially looking for HIV positive patients who develop the kala azar disease even if they are on antiretroviral therapy. Here in Ethiopia we have quite a few cases,” says Aderaju. “We monitor patients for a minimum of three months and up to two years. The aim of the study is improving our understanding of the disease and developing better prevention methods”.
Only a few institutes or pharmaceutical companies are investing time and money in research into kala azar, with the consequence that very few new drug treatments are being developed. Kala azar primarily affects people who cannot afford to pay for the drugs, thus representing an unattractive market for drug companies. Kasaye is one of the currently 325 patients enrolled in the study. “I know many people who have kala azar and I have first-hand experience of how it can affect a person’s life. I want to contribute to the elimination of the disease in Ethiopia.”
MSF has been providing up to date screening and treatment for complicated kala azar co-infected patients with HIV Aids and/or TB in the Amhara Region of Ethiopia since 1997. The Abdurafi project also offers treatment for snakebites – another neglected tropical disease - and provides support to emergency referrals.
ABOUT THE STUDY
PreLeisH (Predicting Visceral Leishmaniasis in HIV Infected Patients) is an observational prospective cohort study launched on 11 October 2017 in Abdurafi. The study investigates the asymptomatic period preceding the onset of active visceral leishmaniasis (VL) in over 1000 HIV‐infected patients over a period of 4 years, as an avenue to develop an evidence‐based screen and treat strategy to prevent progression to active VL.
PreLeisH is implemented in a collaboration between MSF, the Institute of Tropical Medicine Antwerp (ITM), the University of Gondar and the Ethiopian Regional Health Bureau in Amhara. The unique context in the north-western Ethiopian lowlands of a very high HIV/VL co-infection rate provides unique opportunities for research on management of HIV/VL. MSF is the only actor in the region with access to patients as well as capacity to do clinical research.
In the absence of alternative research possibilities in South Sudan (due to insecurity) Abdurafi has developed into a unique centre of excellence for HIV/VL treatment and, over the last few years, MSF has established effective research collaborations with ITM, DNDi and the University of Gondar. Over the past 17 years MSF has carried out 10 kala Azar studies in the Amhara Region of Ethiopia, mainly focusing on HIV/VL co-infection. The impact of these studies has been substantial. They have resulted in policy changes at the national and international level and have driven WHO recommendations and international research agendas.
ABOUT DNDI
DNDi (Drugs for Neglected Diseases Initiative) is a drug research and development organization that focuses on new treatments for neglected diseases, notably leishmaniasis, sleeping sickness, Chagas disease, malaria, paediatric HIV, and specific helminth infections.
The current pharmatheutical industry is market oriented, which leads to the high price of essential treatment solutions for certain diseases. DNDi advocates for enhanced political leadership, sustainable financing, and sound public policies that will encourage greater needs-driven R&D.





Leave a Comment