Stories from the Field in the Time of Pandemic
The pandemic has greatly increased medical needs in various places where Médecins Sans Frontières (MSF) teams have been working and brought new challenges in deploying field staff and supplies alike. Despite these layers of challenges, it was incredible to see our dedicated frontline staff in action to keep our medical programmes running while supporting local COVID-19 response. Amongst these frontline staff, there are three voices from our region to tell their stories. They carried on providing medical humanitarian care to another place and made a difference albeit a bumpy road in the time of pandemic.
From Malaysia, making a difference in Hong Kong

“ Many people were frustrated when they had lost their jobs or housing due to the pandemic. They abandoned their health in order to live a life. Our colleagues worked hard to persuade them that good health is the key to living a better life and begin again.”
Malaysian nurse Eliza Chang joined MSF in August 2018, and became part of the emergency response team working in Hong Kong from the very beginning of the project. At the start of the COVID-19 outbreak in Hong Kong in 2020, MSF started by assisting Hong Kong's vulnerable population, such as the elderly, people experiencing homelessness, street cleaners, the visually impaired, refugees and foreign domestic helpers, who are often neglected in the pandemic. We conducted health education and stress and anxiety management workshops for them.
Even as an experienced infection prevention and control health worker, she admitted that the team had to keep adapting the response through trial and error at the beginning. “Hong Kong was the first place in the world where MSF launched a COVID-19 response project. The extreme urban context is very different from where MSF usually works, so we had to adjust our way of responding. Due to the social restrictions caused by the pandemic, we were not able to conduct face-to-face activities and had to move them online, so it was harder to gauge the responses from our participants.”
“At the same time people in this urban society are also exposed tofake news, rumours and incorrect information that spread quickly throughout communities, and this leads them to challenge our information,” says Eliza.
In addition to health and mental wellbeing promotion, Eliza and her teams had also worked with a local NGO from June to September 2020 to support the homeless by providing free temporary shelters and medical consultations. "The homeless may have more difficulty in implementing preventive measures and accessing medical care, and any single case could develop into a community outbreak if those measure are not taken. It is crucial to inform them how to do the prevention and help them to protect themselves.” The medical team also used MSF's field experience to develop a medical tracker for them, and made sure they were reconnected to the local health system so that they could receive long-term and sustainable medical care.

“Many people were frustrated when they had lost their jobs or housing due to the pandemic. They were living ‘a hand-to-mouth existence’, with the uncertainty of not knowing what the future would bring. They abandoned their health in order to live a life. Our colleagues worked hard to persuade them that good health is the key to living a better life and begin again.” Eliza was glad that team's effort helped to boost these people’s determination to pursue better health when they were constantly and closely followed up. They felt more relaxed knowing there were people who cared about them and had support services available when they were in need.
From China, making a difference in Iraq

“When we made every effort but the patients still died, I felt so powerless and couldn’t help questioning myself. But the local colleague told me that before our arrival, they had to face the plight of nearly 100% mortality. After we started this project, the situation had changed a lot. These words encouraged me at that time.”
Liu Yiyun is an ICU doctor from Shanghai. In October, 2020, she went to Al-Kindi hospital, Baghdad, Iraq for her first mission with MSF. Despite her nine years’ experience, she faced new challenges in Iraq.
In Shanghai, Liu Yiyun and her colleagues would take care of 12 patients in an ICU. However, in Baghdad, she and the other ICU doctor, as well as three or four local doctors in each shift would take care of 24 patients with severe or critical symptoms of COVID-19. She also needed to provide classroom and bedside training to local health workers who had no ICU experience.
Even though Yiyun received a lot of briefings, she was still somewhat daunted when she arrived in the Al Kindi hospital for the first time. Health workers only had limited equipment and were not allowed to use tracheal intubation, which is very common in the ICU, but which presented risks in the COVID-19 epidemic. That means patients with severe or critical case could only receive limited support. Under the infection prevention guidelines, health workers must replace their masks every 6 hours. But in the most difficult period even KN95 masks were almost used up and sometimes people had to wear the same mask for whole day.
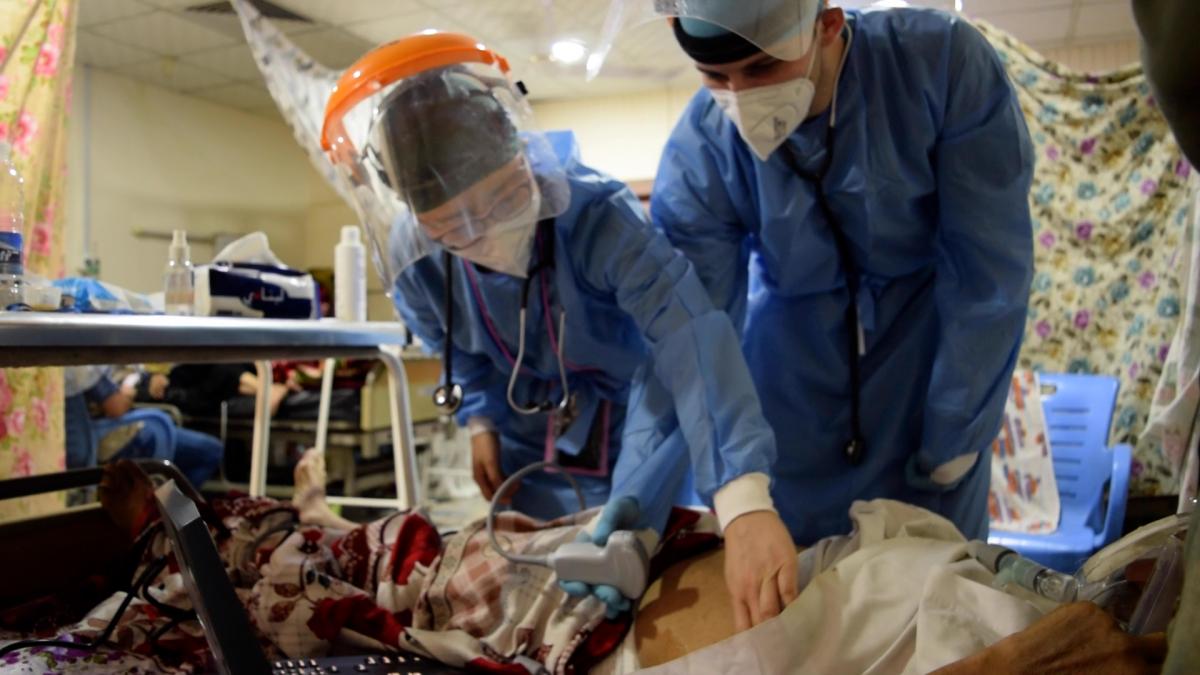
Most of the patients there were over sixty. Many of them were over-weight, accompanied by chronic diseases such as hypertension, diabetes or heart disease, due to the local preference for high-fat and high calorie diet. And the problem of antibiotic resistance is also very serious because of abuse of antibiotics. The delay in getting to hospital was another issue, Yiyun said. “Many of them have stayed at home for two weeks, or went to other clinics when they suspected that they had got COVID-19. After arriving in our hospital, some patients had serious secondary infection, septic shock and even organ failure. Many could not be saved.”
In the first month of Yiyun’s stay in Iraq, it was difficult for her to accept the high mortality rate in the ICU ward. “When we made every effort but the patients still died, I felt so powerless and couldn’t help questioning myself. But the local colleague told me that before our arrival, they had to face the plight of nearly 100% mortality. After we started this project, the situation had changed a lot. They were very grateful for what we had done. These words encouraged me at that time.”
Those local doctors were diligent and eager to learn. They paid attention to Yiyun’s work all the time, as they wanted to learn more to save their people. Yiyun witnessed that through a collective effort, the ward got better equipped and her local colleagues made rapid progress. In October, the mortality rate dropped to 80%, then 60% in December 2020, when the new building designated to treat COVID-19 patients inside the hospital, with single rooms and adequate ventilators was brought into service.
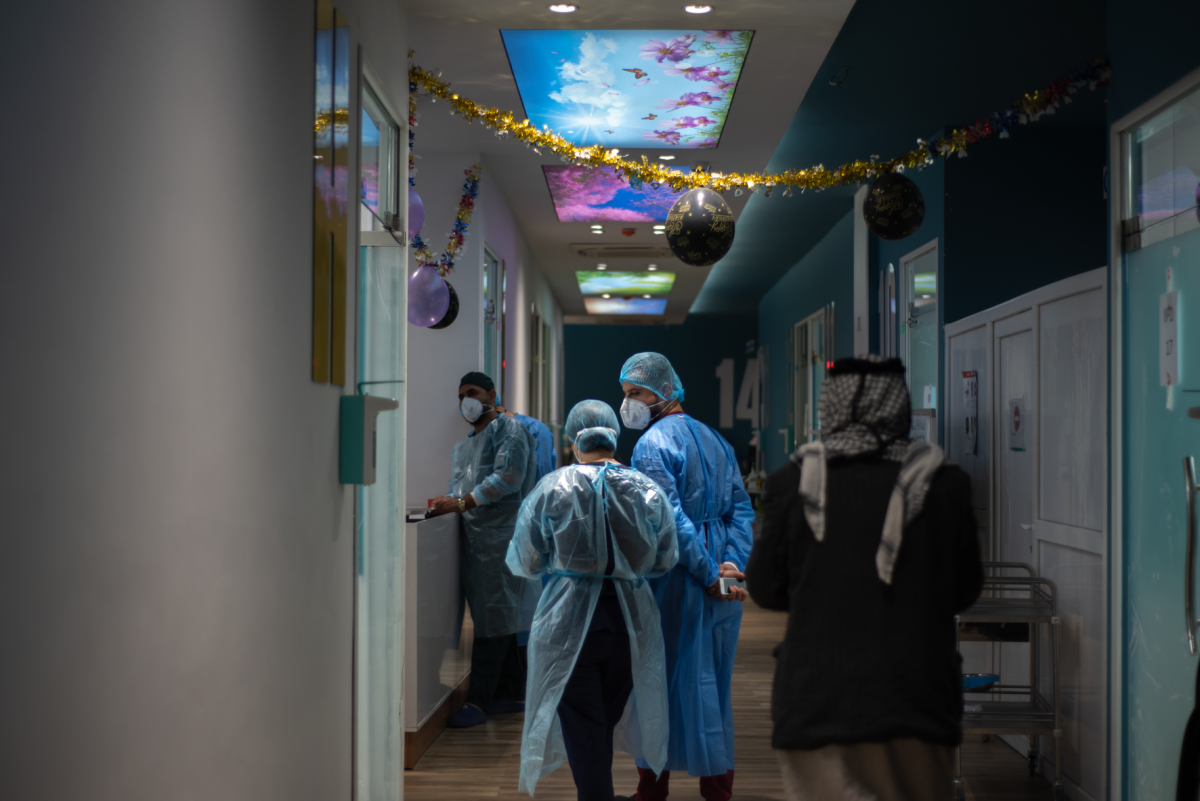
From the Philippines, making a difference in Indonesia

“The frontline health workers would of course be worried about getting infected, but this did not stop them from coming and continuing to work though, unless the health centre itself was forced to be closed for days because of staff testing positive.”
Filipino doctor Roderick Embuido has been with MSF for 12 years and was appointed as the medical coordinator for MSF in Indonesia in November 2020. His main role is to define the medical strategy together with the team and ensure its implementation, modifying the approach according to changes in context and needs.
It was really challenging to implement programmes fully in areas with limited resources, despite an abundance of qualified and skilled people. “The staff understand the importance and the need to implement the programmes, but it’s difficult for them to do it as well as they would like because of the workload and conflicting priorities,” said Roderick.
One of the biggest problems for him was ensuring the protection of MSF staff while providing support to the patients and vulnerable communities, including other health workers in the front line of the pandemic. “We had to ensure our own protection while taking care of other patients, not just COVID-19 patients,” Roderick explained. “The frontline health workers would of course be worried about getting infected, but this did not stop them from coming and continuing to work though, unless the health centre itself was forced to be closed for days because of staff testing positive.

Roderick also pointed out that MSF’s key focus in Indonesia was adolescent health. The large adolescent population in Indonesia was prone to physical and mental health issues even before the pandemic. These were aggravated by the closing of schools and restricting them to their houses, limiting their social interactions.
Although there was an urgent need for locals to fight against the pandemic and improve general medical conditions, Roderick said, the will to fight was fading. “Based on observations in the two specific locations in Indonesia where MSF is working (DKI Jakarta and Banten) people are experiencing a growing fatigue from the prolonged pandemic and health restrictions.”
MSF has been supporting the local response through health promotion and community engagement to increase awareness of the pandemic and the need to follow health protocols. But the community has grown complacent because of fatigue from all the restrictions, the rollout of vaccination in the country and the many false bits of information spreading on social media.
The care for non-critical cases of COVID-19 is not very complicated. Indonesia has competent medical professionals that are able to manage them and has also trained a group of young doctors and medical practitioners on COVID-19 response. MSF, together with the Indonesian Doctors Association, ran one of these courses in 2020. Roderick is still concerned though. “I think the challenge will be more on the volume of patients and whether eventually the health system will be able to handle all of them at the same time.”




