Encouragement and frustrations



May 18, 2015
Awien is a twelve-year-old girl. About a year ago, she started to feel pain in her right loin. Her family took her to many doctors, and all of them said Awien was suffering from urinary tract infection and put her under endless cycles of antibiotics treatments. A year has gone, but she did not feel any better and the pain even extended to her right abdomen. Her family has sold all the assets i.e. cows, in order to pay off the enormous medical expenses.
Awien was sent to our emergency room one day. After thorough clinical examination, I knew her condition was not optimistic. She was having fever, her racing heart beat reached the limit and she appeared to be in the state of septic shock. As I examined her abdomen, I found there was a big mass from her right abdomen to loin, which resulted in a severe pain and signs of peritonitis.
According to her clinical condition, the mass should be a type of abscess, and the source was most likely from acute appendicitis, ascending colon infection, right kidney infection, or tuberculosis infections of the abdominal cavity.
No matter where the source was, Awien's condition was quite critical. We gave her antibiotics injection and then arranged an urgent surgery. The surgery had many uncertainties, which include resection of the intestine, formation of stoma (i.e. artificial anus), and also resection of the right kidney. These were all considered as surgeries with very high risk here in our facility. Because we had no laboratory tests, we were not even able to perform renal function test. We could only check the level of hemoglobin and blood glucose. The operating equipment was also considered to be very basic. Thus, we had to explain carefully every possible operative risk before her family signed the surgery consent form.
As the surgery began, I cut open the abdomen and confirmed the mass was from the right kidney. The mass began to have pus spillage, contaminating the abdominal cavity, which explained the sepsis and peritonitis observed clinically. I cleared all the pus straight away as to avoid the spread of contamination. Shortly after, more than one liter of pus had been sucked. Then I examined her right kidney, I was very shocked to find a tumor. It was as big as a fist, as tough as a bone, and was the source of that one liter of pus. Since we did not have any pathology facilities, it was really difficult to distinguish the tumor nature (benign or malignant). But fortunately, her left kidney was completely normal and there was no sign of cancer spread within the abdominal cavity. Even in the worst scenario that the tumor was cancerous, if it would be completely removed, then the chance for Awien to recover would greatly increase. Hence, I decided to remove the right kidney. After two hours, the whole right kidney together with the tumor were resected.
Awien's rehabilitation was satisfactory. The fever was gone quickly, and the mass and pain in her abdomen that had bothered her for a year also disappeared. Since she was left with only one kidney, we taught her family about kidney care, for example to avoid drugs that would damage the kidney, to drink plenty of water to minimise the chance of having urinary tract stone. Unfortunately, this country lacked clinical oncologist, so even if the tumor was malignant, Awien would not have access to chemotherapy. In any case, we have done our best. We just hope that tumor will never come back. A week after the surgery, she was discharged with a relaxed smile.
It was definitely joyful when we see the patients to be discharged in good health, but sometimes, it could be very frustrating while you were handling deadly condition.
One night, we received an injured man from a traffic accident. He was in coma when he was delivered to the hospital. His left leg had bad open fracture. I temporarily controlled the bleeding on his wound and then began to deal with the most fatal problem, which was the intracranial hemorrhage. Although there was no obvious wound on his head, his pupils were significantly enlarged with different sizes on left and right, and the reaction to light became weak, implying a high possibility of intracranial bleeding. If the blood was not promptly drained, it would increase the intracranial pressure and become life threatening immediately. Therefore, I decided to bet on a bold note by performing burr hole surgery (drilling holes in the skull)!
It was not slightly excessive to call it bold.
First of all, it already took more than one hour for him to be transferred from the accident scene to our hospital, so the golden hour had passed. And due to our lack of CT scan, we would only be able to guess or assume the location of haemorrhage. Besides, if he was bleeding severely he might then need a much more complicated craniotomy operation (opening and removal of part of his skull bone), but we did not have the precision surgical instruments nor the intensive post-operative care here, thus it was absolutely impossible to succeed with these basic facilities.
However, burr hole surgery was his only hope. No matter how slight the chance to succeed, I would not give up this hope.
I asked my nurse to send an orthopedics instrument set. After choosing the location, I cut open his scalp, and use an instrument to drill through his skull bone slowly. It took me quite a lot of effort to drill two holes, and a lot of haemotoma was drained from the right side, which was a good sign as it might help relieving the intracranial pressure.
Nothing much we would do beyond this point. We waited and waited and he continued to stay in coma. Very sadly, he passed away in about three hours.
If we were in Hong Kong, he might have a better chance to survive with the much better medical facilities.
Sometimes, it is not the deadly disease which depressed us, but the ignorance of the local people, which could be extremely frustrating.
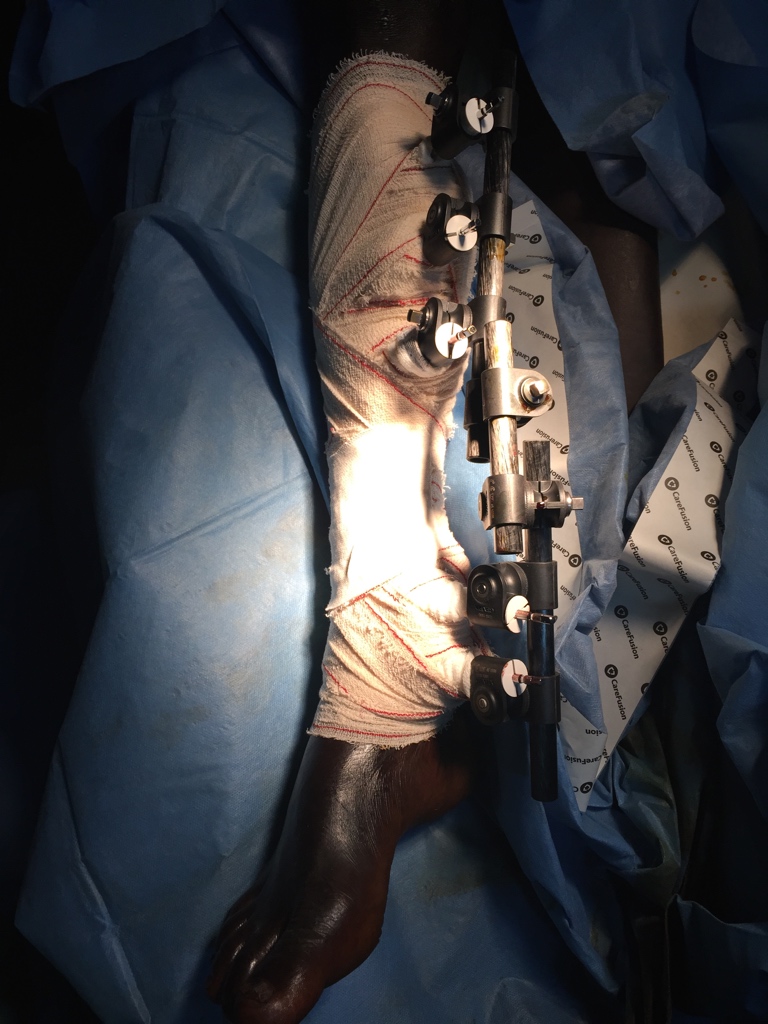
Also caused by a traffic accident, a guy in his twenties broke his right leg when he fell off from his motorcycle. When he was sent to the hospital, he was in extreme pain. The two bones in his right leg were completely fractured and separated, with only fleshes connecting the two sides. Tthe bones could move and even form a 90 degree angle, yet luckily his vessels and nerves seem to be intact. Since the fracture was very unstable, casting with plaster of Paris was not an ideal way to manage it. Hence, I suggested him to have an operation, using external fixator to stabilise the fractures. It would be removed in about two months upon recovery. Since we knew the locals were very into dark magic, particularly for bone fractures, we explained carefully to the patient and his family, and they all agreed to proceed to the surgery.
The surgery went smoothly and the outcome was also satisfying. His pain largely receded. As I explained to his family, I emphasised that he had to avoid weight bearing on his right leg and it would recover in about two months. The whole team was delighted with his recovery.
On the fifth day after the surgery, I received a call from the ward, saying the patient requested for discharge. As I got there, I found out among his relatives, one of them was a local bone healer, or what they called witch doctor. He said the fixation would not heal his leg and he should rely on his dark magic. The witch doctor asked him to leave the hospital and then receive treatment from him, which of course, would cost him a few cattle.
I tried to explain to them patiently and also drew a few pictures to explain the logics behind the surgery. His family agreed to stick with our original treatment, yet the patient himself chose to believe in the witch doctor, either because he was really into dark magic or he believed the treatment would be better if it came at a cost.
We did not have any choices but removing his fixator. It took around 5 minutes to discard those, while we spent over an hour to put it on. The team effort went disappeared as the screws went unscrewed.
As they left the hospital, I gazed towards his leg, it was wrapped with some tree branches by the witch doctor which were bending with the wind. It was in fact quite hilarious. We hope no matter what his next treatment would be, it would not induce any complications nor result in any amputation.
A few weeks later, the miracle girl Awek came back to our hospital for follow up consultation. She was the girl fell from the mango tree. She has been recovering way faster than I expected. She was so energetic, running and jumping around. After a period of iron supplement tablets, her haemoglobin level raised to above 9, which was near to normal. Everyone in the team was so delighted to see her recovering so well.
Her father told me a story: a few years ago, Awek’s elder sister also fell from a mango tree, and was injured like Awek did. He brought the daughter to the local witch doctor, who gave her some treatment. Sadly yet, she passed away soon afterwards. Therefore, when Awek was injured he decided to bring her to us, the MSF. He asked, if he brought her daughter to us at that time, would she survive? Of course I could not answer. But I truly wish that, the local people do not need to learn from pain anymore, and do not need to trade life with ignorance.
My mission in South Sudan was filled with encouragement and also some frustrations. As my mission came to the end, I want to apologise to my patients in Hong Kong, as I would not be able to help you in person when you needed me. Yet fortunately, I have many trustworthy partners to take care of you when I was away. At the same time, I want to express gratitude for all of your support, as you understand, we, the MSF team, are probably the only hope for these underprivileged people in the area.
Greatly appreciated!
Thank you very much!






Leave a Comment