Mission Accomplished!

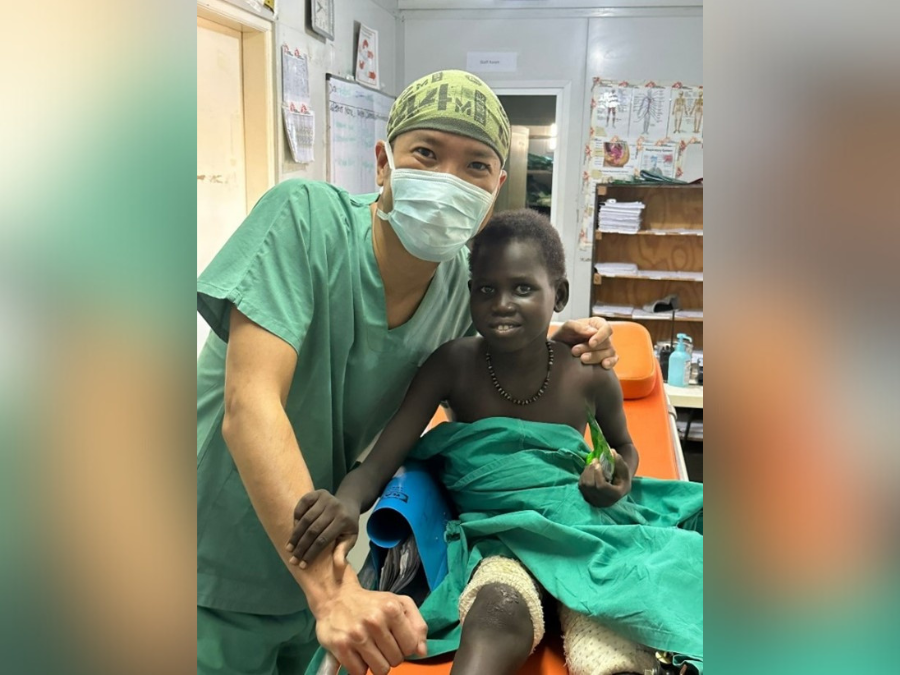
Nyanhial, the 8-year-old girl from Sudan who had a fractured thigh bone resulting from a car accident, successfully undergone fixation surgery in the end of June. Since then, we brought her to the operating theatre and cleaned her wound almost every day. Finally, the wound became clean, and inflammation was greatly reduced – the girl was ready for the next step: a skin graft surgery!
Nyanhial's wound covered nearly the entire front of the thigh, measuring approximately 20 x 40 cm. Given its size, the surgery required precise execution.
Skin grafting can generally be categorized into two types: full-thickness and split-thickness skin transplantation. The principle behind the two procedures remains the same - removing healthy skin from the patient and transplanting it to the wound, which aims to stimulate wound healing.
In Nyanhial's case, a split-thickness skin graft was necessary. This type of graft is good for covering a large area while the donor site wound could heal itself more easily. To increase the area of coverage, we use a special machine to “mesh” a skin graft, creating small holes in the extracted skin and allowing the skin to be stretched. The mesh allows fluid to leak out, reducing the risk of infection. Once there is bacterial infection, it’s very likely that the transplanted skin cannot thrive.
Therefore, we spent over a month to clean Nyanhial's wound as much as possible. In early August, we were finally able to perform the skin grafting. Using an electrical dermatome, I cut out two long and thin strips of skin from Nyanhial's healthy right thigh and then carefully meshed the skin with a machine.
Our meshing machine was old and dilapidated, largely discounting the meshing effect. Therefore, one day before the surgery, we thoroughly check the machine again, identifying its problems and coming up with solutions.
Fortunately, the meshing effect this time was very ideal, and the small holes were made neatly.
We then put the two strips of meshed skin on Nyanhial's wound on her left thigh and stitched the wound up. Mission accomplished! The team in the operating theatre smiled with satisfaction.
A week later, it was time to assess the results during the first dressing change and wound assessment.
As we carefully removed the old dressing, the tension in the room was palpable. When the last layer of gauze was taken away, my colleagues exclaimed in their local language. They said, "Goa Long!" (meaning “very good”).
I was extremely pleased with the overall outcome of the skin graft. If I had to rate this operation, I would undoubtedly give it a solid ten!
My homecoming day is approaching. Nyanhial's remaining treatment will be entrusted to another experienced surgeon from Hong Kong. Once the girl’s fracture and skin are fully healed, the external fixator will be removed, and she will embark on a long and challenging journey of rehabilitation.
I firmly believe that in the near future, Nyanhial will regain her ability to walk normally and return to a normal life.
I have fulfilled the promise that I make to her, and it serves as a perfect conclusion to this remarkable journey!





Leave a Comment