Ukraine: A year in destruction
by Christopher Stokes, MSF head of mission in Ukraine

On 24 February 2022, we awoke at night to the rumble of distant explosions, the sound of fighter jets dropping missiles on Kyiv, and the astonishing news that Russia was invading Ukraine.
None of us knew what to expect. I had arrived four days previously to try to establish a network of contacts who could help us work if there was a major escalation in conflict. MSF first worked in the country in 1999 and had been responding to the fighting in eastern Ukraine since 2014, but in truth, we were poorly prepared. .
For many aid organisations, and indeed a lot of Ukrainians, the denial that had preceded the invasion made way to disbelief and, for ordinary civilians, a sense of impending doom mixed with anger. Numerous NGOs left the country entirely, exacerbating the subsequent need for a massive scale-up in the humanitarian response.
In those first days, between 10 and 15 million people fled their homes. Remarkably, however, we did not witness any panic or looting. No flights were leaving, as all airports, both civilian and military, had been hit by Russian missiles at the outset.
This was not the first time I had worked with MSF in a conflict zone, nor the first time I had witnessed the start of a major war. However, inter-state invasions are rare (for example, the US invasions of Afghanistan in 2001 and of Iraq in 2003) and the intensive phase, although bloody, is usually short-lived. The situation in Ukraine has not turned out that way at all.
We moved from Kyiv to Lviv and started redefining and rebuilding our medical assistance from there. Few international staff felt safe enough to stay so we launched our activities mostly with our Ukrainian colleagues, who stepped up to the challenge even though they were all now displaced, and having to find a roof for their families in safer parts of the country.
The next question was: what would be the most effective course of action in such a fast-moving war? Where could a medical humanitarian NGO make the biggest difference?
It quickly became clear that civilians would not be spared. Families leaving Kyiv were killed on the roads leading east and south, as tanks opened fire on sight without warning. We therefore set up programmes to help hospitals deal with mass-casualty influxes and war trauma, a highly specialised field distinct from ‘ordinary’ trauma such as road traffic accidents.
We also made emergency orders to resupply hospitals so they could cope with the increased trauma workload – a standard approach to war in a middle-income country with a solid specialist healthcare infrastructure. The idea was to help an existing system cope with an extraordinary workload.
However, Ukraine had been at war, albeit a more geographically restricted one, since 2014. It was better prepared than most healthcare systems would be. Yes, some local doctors and nurses left with their families, but the majority stayed.
By mid-March, we decided to try something new, as some noticeable gaps in healthcare were appearing. One thing was clear: the railways were still working, and remained a key form of transport. Many people, including those with wounds and other vulnerabilities, were travelling by train, usually westwards, away from the heavily shelled eastern and central regions. But the regions and their hospitals were not used to these long-range transfers.
Late one evening, in a meeting with the focal points from the Ukrainian national railway company, Ukrzaliznytsia, in Lviv, I proposed using modified “‘medicalised”’ trains to evacuate patients to the west. They jumped on the idea and recalled that something similar had been done during the Second World War.
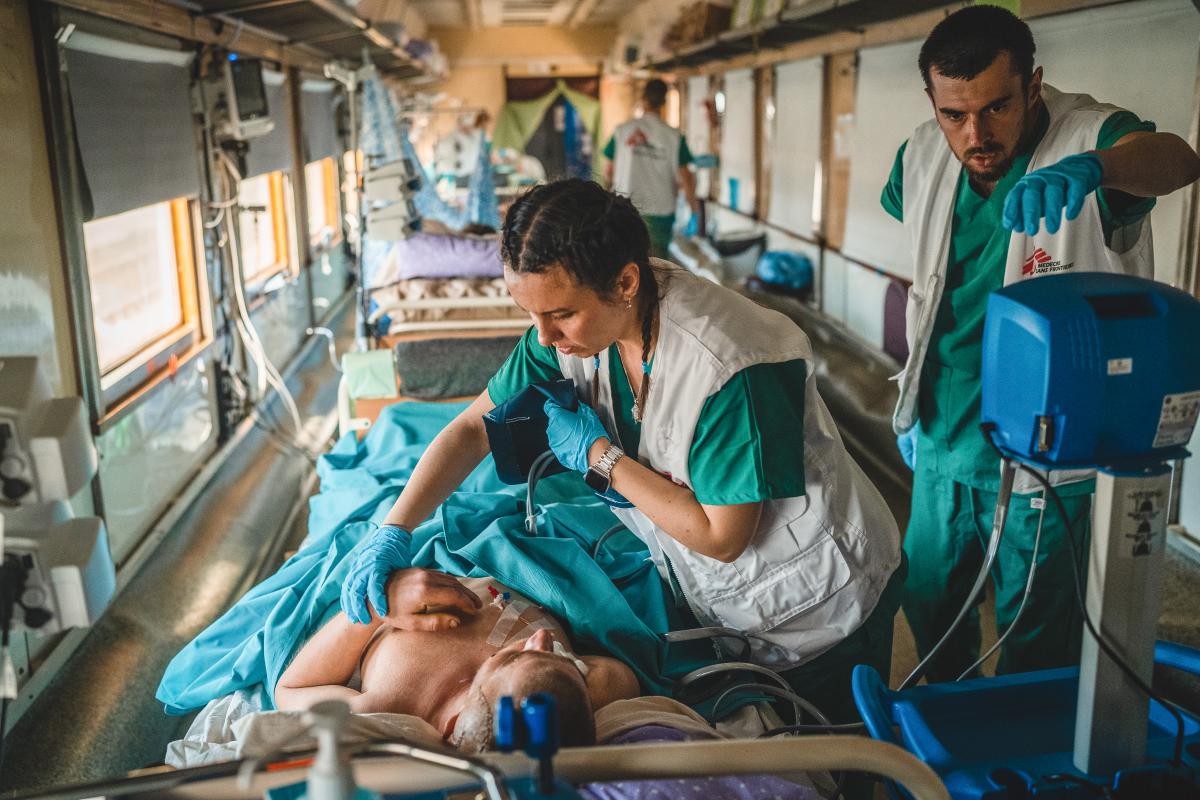
They set about stripping wagons in the railway depot, as we sent medical equipment and technicians to prepare them for intensive care, complete with oxygen concentrators and autonomous electric power. We had no idea if the project would work beyond maybe a few rotations at best. By the end of the year, some 2,500 patients had been safely moved across the country over 80 rotations, often at night, with trips usually lasting 24 hours or more.
The war also took a toll on ambulance services, as crews were injured or killed and their vehicles destroyed (notably in Luhansk and Donetsk), while the number of war-wounded patients continued to increase. As a result, emergency ambulance transport became a core component of our medical response in the most war-affected regions of eastern Ukraine, with 50 to 100 referrals a week. Typically, we transferred war-wounded patients from depleted Ministry of Health hospitals near the frontline to the relative safety of Dnipro, where they could receive the care they needed.
In addition, we ran mobile clinics to assist people who had been cut off from healthcare under Russian occupation in Kherson, Kharkiv, Chernihiv, Kyiv and Mykolaiv. As villages and towns were recaptured by Ukrainian forces, we discovered that most of the elderly people who had decided to stay behind or been unable to flee in time had had no access to care or to the vital drugs prescribed to them before the war to manage their chronic conditions.

In Kherson alone, our mobile clinic services covered over 160 villages and towns, offering both medical and mental health support. Often people had survived, but their villages and health centres had been destroyed by bombs or airstrikes, or even looted by departing Russian soldiers.
The extent of the destruction must be seen to be properly understood. It stretches along a 1,000-kilometre frontline and is dozens of kilometres deep on both sides. Not a single village is undamaged. It will potentially take decades to rebuild the country. Families who evacuated have told me they may never return, while those who stayed are still living in shelled-out buildings with little medical assistance beyond short flash visits.
It is important to state that the bulk of assistance here and throughout the country is provided by national authorities, backed by dynamic civil society activists who self-organised from day one. They go where no international organisation dares to, sometimes at great personal cost.
Meanwhile, in spite of prolonged negotiations, Moscow has not granted MSF permission to work on the other side of the frontline, in regions of Ukraine currently under Russian control. This is regrettable, as the situations we have discovered in areas previously under Russian control, lead us to believe that humanitarian access there is a priority. Ukrainians with whom we have been in touch in Mariupol, Zaporizhzhia and Kherson confirm the high level of needs and request assistance.
We can only hope this will change, as the war shows no sign of ending and people continue to suffer the constant stress and danger of daily drone and missile strikes.
Re-adjusting the focus: Our responsibility towards people we photograph
by Jean-Marc Jacobs, MSF International Communications Coordinator and Juliette Garms, MSF Photography project manager
In 2022, in partnership with a major photo agency, MSF published images of a 16-year-old girl who was the victim of rape in the Democratic Republic of Congo. Following widespread criticism, both within MSF and externally, we removed the images from all our platforms.
The controversy sparked a wider conversation about the protection and visual representation of people in the care of MSF, and the circulation of such imagery for editorial, fundraising and commercial purposes.
Bearing witness to the plights of communities we support is fundamental to the mission and identity of our organisation, and over the years, visual stories, commissions and collaborations with media and photo agencies have played a key role in helping us to do this. Along the way, MSF has contributed to shaping norms and establishing standards in the humanitarian photography field. Today, we must question these very same norms and standards.
Photography is a powerful way to inform, provoke and create a sense of empathy. But as a medical organisation, our primary duty must be to protect the privacy, dignity and agency of patients in our care. The medical principle of “‘doing no harm”’ cannot be sidelined when depicting people in their most vulnerable moments, in order to raise global awareness and funds.
We must acknowledge that we have not always lived up to this principle. How did images of suffering bodies become so ubiquitous and to what extent has MSF contributed to normalising the pain of others? Did we forget to ask ourselves: how would I feel if the person in this photograph was my son, my father, my sister?
This excessive display of suffering is both unjustifiable and unnecessary. As a global NGO, and as individuals, we must reflect on how our worldview and choices are influenced by historical power dynamics, and to what extent they have created deep-rooted biases.

MSF has been called out on images of our patients on news and photo agency websites, for which we do not hold the copyright. When photos of our patients are taken during a media visit and posted on a news agency platform, both MSF and the agency instantly lose control over their circulation and use. We must therefore acknowledge that, by prioritising high public visibility, in a context of increased marketisation of the news sector, we have contributed to the over-exposure of people in our care and facilitated the wide dissemination of sensitive, intrusive and sometimes disturbing images.
While MSF does not profit from these images, news and photo agencies do; many images are available to buy on their websites. They can also be found on social media, and in books and internal publications. In a digital era, images can stay online for decades. Did all these photos need to be taken? No. Could we have used and disseminated them differently? Yes.
In 2022, heads of communications across the MSF movement recognised our shortcomings and committed to do better. Dr Christos Christou, MSF’s International President, acknowledged that mistakes had been made and reaffirmed that “MSF’s ultimate responsibility is to protect the health and well-being of the people we seek to assist”.
Pathways for change
Our drive to implement changes in visual representation converges with our commitment to produce content in a more inclusive, respectful and accurate manner for communications and fundraising, in line with new guidance we produced in 2021. Concrete actions are being taken at different levels of the organisation; all part of a critical self-inquiry period that will help redefine how we produce stories.
Back in 2021, we launched a project to investigate the thousands of images in the MSF archive. We started by reviewing photographs according to several ethical criteria, including stereotypes, lack of dignity, disturbing or offensive content, protection of minors, security risk, medical practices and nudity. By the end of 2022, this process had helped us identify 10,000 potentially problematic images. The most sensitive images are now hidden from the database for most users, while the remaining ones carry a specific warning in their captions.
In 2023, this preliminary work will be refined by a panel of internal and external advisors, comprising photography and child protection experts, curators, academics, ethicists, patient activists and first-line medical workers. The panel will review a set of these problematic images and make recommendations, which we will apply to the full media database and use as a critical guideline to direct how we collect, store and use images in the future.
Regarding images hosted outside our own media database, we have had a first round of interactions with news and photo agencies to gain an understanding of their ethical standards and content management. Initial findings indicate loose editorial control and high automation of content upload.
As a result, we are taking steps to amend our collaborations with these agencies and asking them to remove or restrict distribution of certain sensitive images. We are also reviewing our standard contracts with external photographers, especially clauses related to reselling images taken during their assignments to external media.
These are complex issues that involve everyone who works with us. Real cultural change will require ownership at all levels of the organisation. We are therefore engaging with a wide variety of people within MSF through surveys and workshops, so that they can contribute to help define how we work with imagery, and also share their challenges, opinions and experiences.
The notion of informed consent and agency will be at the core of these considerations. The process will involve listening to community-based staff to better understand the needs of patients being represented, including their sometimes-strong desire to speak out about the situation they are facing. These conversations will help determine whether a photo should be taken, how it might be used and for how long.
The outcomes of these internal and external consultations will be analysed in 2023 and will serve as the basis for clear decisions on how we produce, store, commission and disseminate images. Inevitably, there will be difficult conversations and disagreements. However, there is a consensus on the fact that the dignity and integrity of our patients should prevail over all other considerations. Even if it means snapping and sharing less often.
We owe this collective change to the people to whom we provide care.




